Of the existing literature, journey mapping techniques are described mainly in process papers, outlining their potential utility in observing healthcare delivery and patient outcomes. As medical journey mapping is still in its infancy, there is an absence of literature exploring implementation. Integrating diverse components of the patient healthcare journey provides a holistic perspective of the relationships between the different elements that may guide directions for change and service improvement. Medical journey mapping involves creating narrative timelines, by incorporating markers of the patient experience with healthcare service encounters. It is gaining increasing recognition for its ability to organise complex multifaceted data from numerous sources and explore interactions across care settings and over time. Journey mapping is a relatively new approach in medical research that has been adapted from customer service and marketing research. The utilisation of journey mapping has the potential to address these inconsistencies and to our knowledge, this research is the first of its kind. This has subsequently translated into significant variability in palliative care research and limitations in applying international evidence to clinical practice. However, differing patient, illness trajectory and clinical factors have resulted in inconsistencies in the degree of care provided. A key area of medicine able to address these issues is palliative care.Ĭentral to optimal delivery of palliative care is timely initiation. There is an urgent need to ensure timely proactive medical care, effective and efficient resource deployment, while averting unnecessary, often distressing, emergency department (ED) presentations, admissions and conveyor belt medicine. Patterns of healthcare utilisation are evolving in response to the ageing population and increasing burden of chronic disease. This is particularly significant as machine learning and big data is increasingly applied to healthcare. This unique qualitative study noted many promising applications of the journey mapping suitable for extrapolation outside of the palliative care setting as a review and audit tool, or a mechanism for providing proactive patient-centred care. Through these journey maps, participants were able to identify barriers to effective palliative care and opportunities to improve care delivery by observing patterns of patient function and healthcare encounters over multiple settings. Journey maps provided a holistic patient-centred perspective of care that characterised healthcare interactions within a longitudinal trajectory. Our thematic and Delphi analyses were congruent, with consensus findings consistent with emerging themes. This study utilised a qualitative mixed-methods approach, incorporating a modified Delphi technique and thematic analysis in an online questionnaire. Sixteen maps were purposively selected from a sample of 104 consecutive patients. MethodsĪ purposive convenience sample of specialist palliative care providers from the Supportive and Palliative Care unit of a major Australian tertiary health service were invited to evaluate journey maps illustrating the final year of life of inpatient palliative care patients. Specialist palliative care services were selected as the model to evaluate this paradigm, as there are numerous evidence gaps and inconsistencies in the delivery of care that may be addressed using this tool. 
To determine possible applications of journey mapping in medical research and the clinical setting. 
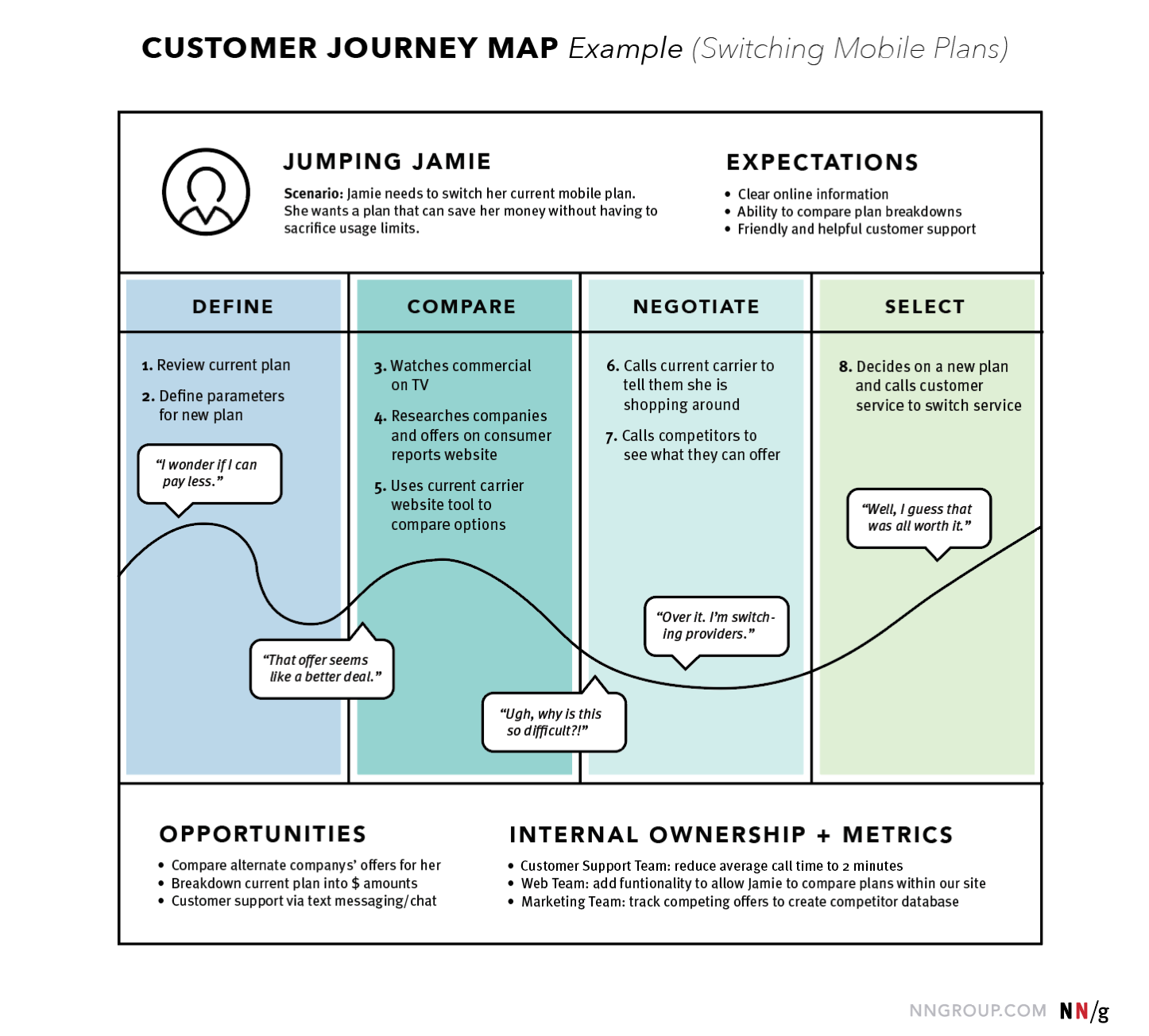
The use of journey maps in medical research is a novel and innovative approach to understanding patient healthcare encounters. Journey mapping involves the creation of visual narrative timelines depicting the multidimensional relationship between a consumer and a service.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
